Medical Plans
low-level alert: Important Network Change

Effective June 1, 2025, mental health counseling is covered at 100% for all Cook County employees and dependents enrolled in a medical plan. There are no copayment, deductible, or cost-sharing requirements, or visit limitations under the plan.
Medical Benefit Plans
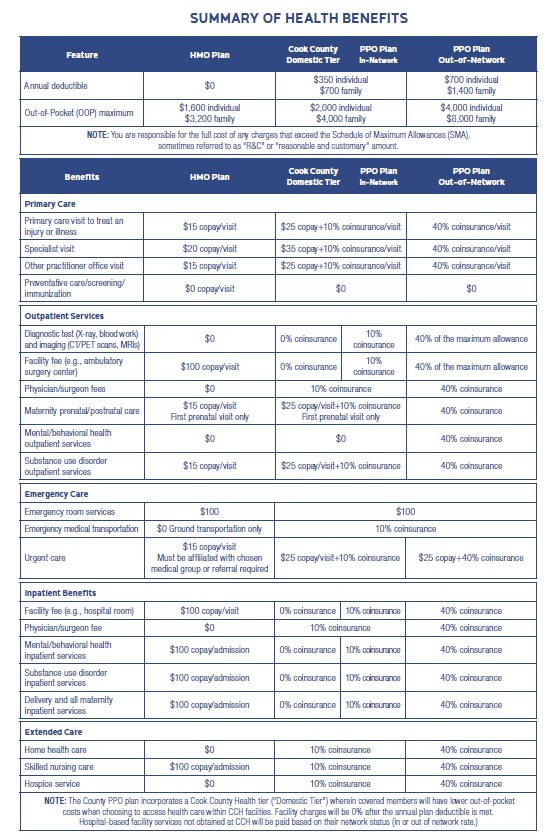
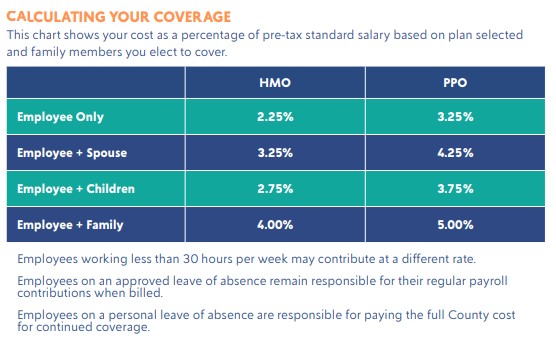
The County offers two medical benefit plans: Blue Advantage HMO and Blue Cross Blue Shield PPO. Please see plan details below.
Group #B03351
Customer Service 1-800-892-2803
Information
Register for BlueAccess for Members
Blue Cross Blue Shield Provider Finder
Documents
BlueAdvantage HMO Certificate
- Group #B03351
BlueAdvantage HMO Summary of Benefits and Coverage
- Group #B03351
2026 Employee Benefits Overview*
Single Sign On Login Steps / Click here to access the Blue Cross Blue Shield Blue Access for Member Single Sign On Webpage
*This benefit guide is intended for informational purposes only and does not constitute a contract or guarantee of coverage. Benefits may change at any time, and employees should always refer to the official plan documents for the most up-to-date information regarding their eligibility and coverage details.
Group #291116
Customer Service: 1-800-960-8809
Information
Register for BlueAccess for Members (BAM)
Blue Cross Blue Shield Provider Finder
Forms
Documents
PPO Certificates
- Group #291116 (2026)
PPO Summary of Benefits and Coverage
- Group #291116 (Plan Year 2024-2025) / #291116 (Plan Year 2025-2026)
PPO Nationwide Program Overview
Understanding Your Explanation of Benefits (EOB)
2026 Employee Benefits Overview*
Single Sign On Login Step / Click here to access the Blue Cross Blue Shield Blue Access for Member Singe Sign On Webpage
*This benefit guide is intended for informational purposes only and does not constitute a contract or guarantee of coverage. Benefits may change at any time, and employees should always refer to the official plan documents for the most up-to-date information regarding their eligibility and coverage details.
Fitness Program Membership Discount
Blue365 Discount Program (save money on health and wellness products)
